Written by
Australian Dog Lover
15:01:00
-
0
Comments
An anaphylactic reaction otherwise known as anaphylaxis is an immediate severe allergic reaction caused by an exposure to a foreign substance.
We have teamed up with Dr Lisa Smart from the Small Animal Specialist Hospital (SASH) to learn more about anaphylaxis in dogs – its symptoms, causes and what treatments are available.
Dr Smart has completed a PhD in Emergency Medicine. Her current research interests include shock, coagulation, fluid therapy and anaphylaxis. She is a specialist in emergency medicine and critical care - i.e. a vet who specialises in treating the most unstable and time sensitive patients - at SASH Central Coast.
What is anaphylaxis?
Anaphylaxis is a very serious and sudden reaction, in which the body becomes oversensitive to a foreign substance. In dogs, the syndrome may present in a variety of forms.
This may affect the cardiovascular system in the form of low blood pressure or have gastrointestinal effects causing vomiting and/or diarrhoea. Other recognised symptoms include the dermatological signs that present in the form of welts and/or itchy skin, or difficulties breathing.
What causes anaphylaxis in dogs?
There are a number of allergies that can cause an anaphylactic reaction in dogs.
From a study that was conducted in Perth, almost 50% of cases presented were caused by insect stings, 4% due to an adverse reaction to medication and the remaining from unknown causes.
Bees, wasps, and ants are among the insects whose venom can contain a variety of chemicals, including toxins and allergenic substances that when exposed to dogs can cause sensitivity.
Due to the allergy of the foreign substance, the anaphylactic reaction is the immune system reacting in defence of the sting, medicine, or other unknown cause. There also may be additional chemicals in the venom of insects that activates the immune system or cause tissue damage.
In this particular study, the median age of the dogs was 1.2 years, however, dogs of any age can be affected.
In this particular study, the median age of the dogs was 1.2 years, however, dogs of any age can be affected.
Dogs may develop the syndrome later in life and anecdotally, it has been noted that subsequent reactions may increase in severity if affected again.
Yet, some pets have an anaphylactic reaction once and then may never again experience the condition. It may be thought that puppies are more susceptible to the syndrome, however, this is not the case.
Puppies, with their playful natures and curiosity, place themselves more often in the proximity of insects. However, one breed that does stand out is the Dachshund breed; there is some evidence that they seem particularly susceptible to insect sting anaphylaxis.
Over the length of the study conducted from 2006 – 2018, the prevalence of anaphylaxis in dogs remained at a steady rate.
What are the symptoms of anaphylactic reaction?
What are the symptoms of anaphylactic reaction?

Recent studies have defined the syndrome involving at least two organ systems ranging from dermatological, respiratory, cardiovascular, or gastrointestinal signs. For pet owners and treating veterinarians, the well-known symptom - changes to skin when a dog is experiencing anaphylaxis - is more easily identified than internal symptoms.
Here are the main signs to look out for if you suspect your dog is experiencing anaphylaxis:
✔️ Vomiting
✔️ Intense bowel movements
✔️ Unsteady movement or wobbling as they are walking
✔️ Shaking or convulsion of the body
✔️ Facial swelling
✔️ Rashes developing on skin
✔️ Welts breaking out on the body
Approximately 75% of dogs with anaphylaxis have changes to the skin, 76% have gastrointestinal symptoms and 69% have changes to their blood circulation (or shock).
Anecdotally, when vets across Australia have discussed these types of cases, there appears to be variation in number of cases seen and the severity of reactions. It is thought that the bees in the Perth region, where this large study was based, are particularly vicious, based on the cases seen in this region.
Variation of signs means that anaphylaxis may be confused with other problems. Moreover, if a dog has a thicker coat, the dermatological symptoms may be more difficult to spot. My future research, in collaboration with Murdoch University, seeks to identify potential blood tests that can assist in diagnosing this problem in the emergency department.
What to do if your dog has an anaphylactic reaction
Symptoms can occur very rapidly and so it is important to seek veterinary advice immediately. Take your pet straight to the vet if you suspect your dog is experiencing anaphylactic shock.
What to do if your dog has an anaphylactic reaction
Symptoms can occur very rapidly and so it is important to seek veterinary advice immediately. Take your pet straight to the vet if you suspect your dog is experiencing anaphylactic shock.
If your dog has been stung by an insect, remove the stinger – you can do this gently with some tweezers. Put the stinger into a container and bring with you to the vet so that they can confirm that it appears to be from a bee. It’s very important that owners don’t self-medicate as this may cause even more stress on the body or delay the trip to the vet.
If your dog has a flat face, such as the Bulldog breed, it is important to keep them calm and cool while travelling to the vet (air conditioning or fan), as they are at increased risk of trouble breathing and over-heating when stressed.
Anaphylaxis in dogs presents differently than other animals and often shows more symptoms. For instance, in cats an anaphylactic reaction may show in the form of trouble breathing, like an asthma attack. Whereas in dogs, it may also affect the liver, the gut and cause abnormal blood flow. In some cases, internal bleeding may occur, and the dog may need a blood transfusion.
One of the areas of the discussion between vets are the use of epi-pens by owners if an anaphylactic reaction occurs at home. However, there has not been enough research conducted to form a substantial conclusion and provide comprehensive recommendations.
What treatments are available?
Anaphylaxis in dogs presents differently than other animals and often shows more symptoms. For instance, in cats an anaphylactic reaction may show in the form of trouble breathing, like an asthma attack. Whereas in dogs, it may also affect the liver, the gut and cause abnormal blood flow. In some cases, internal bleeding may occur, and the dog may need a blood transfusion.
One of the areas of the discussion between vets are the use of epi-pens by owners if an anaphylactic reaction occurs at home. However, there has not been enough research conducted to form a substantial conclusion and provide comprehensive recommendations.
What treatments are available?
Anaphylaxis is an emergency and requires immediate medical intervention. Once a dog is presented at a veterinary clinic, they may receive a range of treatments depending on the severity of the reaction and the cause. The goals of these treatments are to assist with breathing and to administer drugs which will stabilise the pet to minimise additional shock.
An antihistamine injection may be administered and if more acute, the dog may be placed on a drip and given intravenous fluid or adrenaline. The good news is that 58% of dogs go home soon after assessment by a vet and if admitted to hospital, 88% of dogs go home within 12 hours.
Anaphylaxis usually has a great outcome, with very low mortality rate – under 0.5%. Death is usually due to euthanasia if a dog is experiencing severe complications and requires high level costly treatment. This highlights the importance of pet insurance to cover therapies for conditions that are easily treatable.
What is the recovery like for anaphylaxis?
Once dogs have received their initial treatment, they may make a full recovery with the help of treating veterinarians.
Depending on the severity of the case, dogs may have ongoing appointments with the dermatologist and receive immunotherapy to reduce the severity of the symptoms. This may be in the form of vaccines, or immunotherapy, and additional medications to help reduce the reaction from how the body responds if exposed to the allergen again.
Although there are not many options for prevention, pet owners can clear their backyards from insect drawing plants to help minimise the chances of an insect sting.
Dr Lisa & Frodo's Story
I found Frodo, my 4-month-old Gordon Setter puppy, collapsed in my backyard surrounded by flowers with bees on them.
There were multiple piles of vomit around him. He was pale in the gums and having trouble standing.
 |
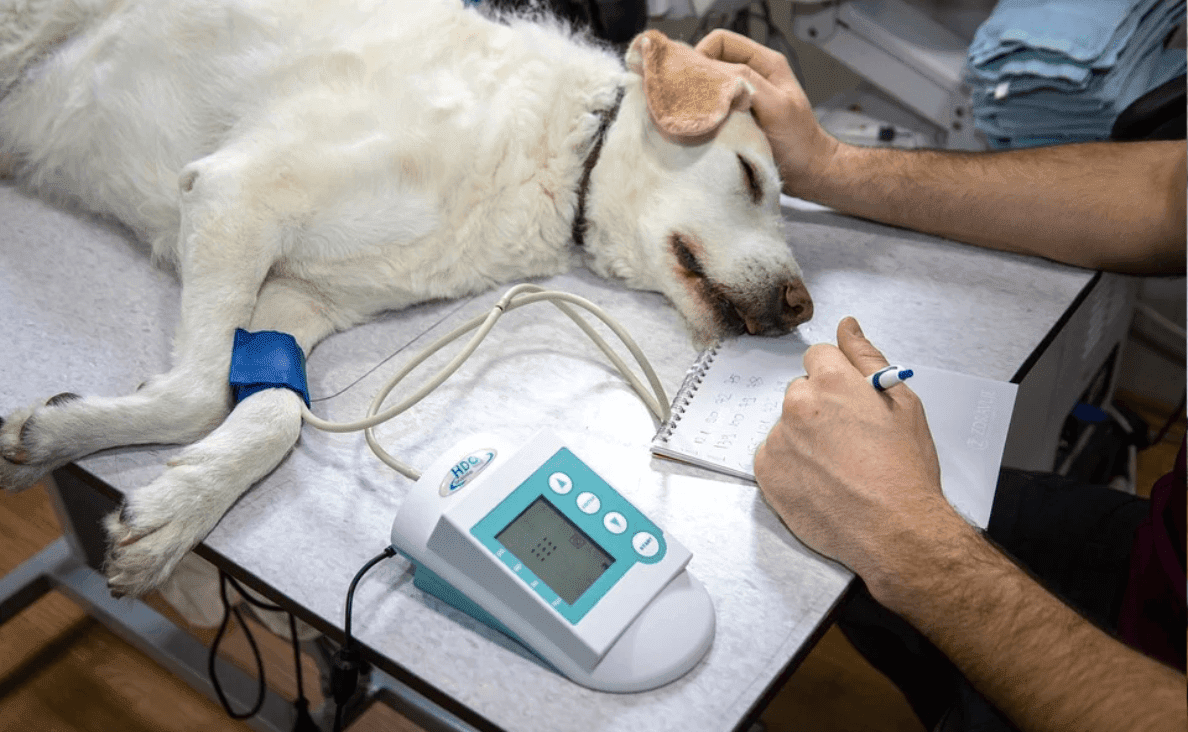
| Frodo being treated for anaphylaxis. Note the puffy eyelids and lips. He is getting fluid through a catheter in one leg and his blood pressure monitored via the cuff on the other leg. |
There he was found to have a slow heart rate and no readable blood pressure on the monitor.
An emergency ultrasound was performed, and he had swelling of his gall bladder in his liver, which is a typical finding in anaphylaxis. He was given an injection of antihistamine.
He then developed a puffy face, and it was clear that he had been stung by a bee.
An intravenous catheter (or cannula) was placed in his leg, and he was given rapid intravenous fluids, also known as a drip, to increase his blood pressure.
After each dose of fluid was given, his blood pressure slowly came up. After three doses, his blood pressure was adequate, therefore an injection of adrenaline was not needed.
Frodo made a fast recovery from that point and went home. He returned to the hospital in a month’s time to see the specialist Dermatology service. They tested him for bee and wasp allergy by injecting small amounts of venom under the skin and seeing if his skin reacted. He reacted strongly to both venoms.
Frodo made a fast recovery from that point and went home. He returned to the hospital in a month’s time to see the specialist Dermatology service. They tested him for bee and wasp allergy by injecting small amounts of venom under the skin and seeing if his skin reacted. He reacted strongly to both venoms.
 |
| Frodo loving life, playing with his buddy Charlie |
He did very well with this treatment.
About 6 months after starting immunotherapy, he was found trying to eat a bee on the ground and developed a puffy lip and swollen eyelids. However, he did not develop anaphylaxis!
He is now 9 years old and has never had another anaphylaxis event, despite being an avid bee chaser. His case prompted my research interest in anaphylaxis, leading to several studies on the syndrome.
He is now 9 years old and has never had another anaphylaxis event, despite being an avid bee chaser. His case prompted my research interest in anaphylaxis, leading to several studies on the syndrome.
written by Dr. Lisa Smart, SASH Vets Central Coast, May 2022 for Australian Dog Lover (all rights reserved).
About Dr Lisa Smart
Dr Lisa Smart completed a Bachelor of Veterinary Science at the University of Queensland in 2003 before undertaking a rotating internship at Queensland Veterinary Specialists and Pet ER.
About Dr Lisa Smart
She then went on to complete a 3-year residency program in Small Animal Emergency and Critical Care at the University of California, Davis, Veterinary Medical Teaching Hospital, and achieved board certification with the American College of Veterinary Emergency and Critical Care in 2008.
This was followed by a move to Perth and almost 13 years spent as Senior Lecturer in Emergency and Critical Care at Murdoch University.
Dr Smart has also recently completed a PhD in Emergency Medicine. Her current research interests include shock, coagulation, fluid therapy and anaphylaxis. She is also currently a teleconsultant for VetCT, providing phone advice to veterinarians treating critically ill patients.
In 2022, Dr Smart joined the team at SASH Vets Central Coast. She is one of the only Criticalists in the region and loves working with the team and referring vets to provide additional high-level care for the pets. You can follow SASH Vets on Facebook: www.facebook.com/sashvets
Related Topics:











